 From smartphones and tablets to laptops and desktop monitors, screens are now part of nearly every hour of our day. While technology keeps us connected and productive, increased screen time has led to a growing concern in eye care: digital eye strain.
From smartphones and tablets to laptops and desktop monitors, screens are now part of nearly every hour of our day. While technology keeps us connected and productive, increased screen time has led to a growing concern in eye care: digital eye strain.
Also known as Computer Vision Syndrome, digital eye strain refers to a group of vision-related symptoms that result from prolonged use of digital devices.
What Causes Digital Eye Strain?
When we use screens, our eyes work harder than usual. Several factors contribute to discomfort:
- Reduced blinking while staring at screens
- Poor lighting or glare
- Improper viewing distance or posture
- Uncorrected vision problems
- Small text or low contrast settings
On average, people blink about 15–20 times per minute. During screen use, that number can drop by nearly half — leading to eye dryness and irritation.
Common Symptoms
You may be experiencing digital eye strain if you notice:
- Blurry vision
- Dry, irritated, or watery eyes
- Headaches
- Neck and shoulder pain
- Difficulty focusing
- Increased light sensitivity
While these symptoms are usually temporary, frequent discomfort can affect productivity and overall eye health.
How Blue Light Fits In
Digital screens emit blue light, a high-energy visible light that may contribute to eye fatigue and disrupt sleep patterns. While research is ongoing regarding long-term retinal damage, many patients report reduced discomfort when using blue light filtering lenses — especially in the evening hours.
Who Is Most at Risk?
Anyone who spends two or more continuous hours on a screen daily is at risk. This includes:
- Office workers
- Students
- Remote workers
- Gamers
- Children using tablets and phones
With remote work and virtual learning becoming more common, cases of digital eye strain have increased significantly in recent years.
How to Protect Your Eyes
The good news: small changes can make a big difference.
Follow the 20-20-20 Rule
Every 20 minutes, look at something 20 feet away for at least 20 seconds. This allows your eye muscles to relax.
Adjust Your Workspace
- Keep screens about 20–28 inches from your eyes
- Position the monitor slightly below eye level
- Reduce glare from windows or overhead lighting
Blink More Often
Make a conscious effort to blink fully to keep eyes lubricated.
Use Artificial Tears
Preservative-free lubricating drops can relieve dryness.
Schedule Regular Eye Exams and Special Glasses
An ophthalmologist can detect underlying vision issues and recommend corrective lenses specifically designed for computer use.
When to See an Eye Doctor
If symptoms persist despite lifestyle changes, it’s important to schedule a comprehensive eye exam. Persistent eye discomfort could indicate dry eye disease, uncorrected refractive error, or another underlying condition.
The Bottom Line
Digital devices are here to stay — but eye discomfort doesn’t have to be. With mindful screen habits, proper ergonomics, and routine eye care, you can reduce digital eye strain and protect your vision for the long term.







 Low vision affects millions of Americans — including many older adults. People with low vision aren’t blind, but because of their vision loss, they may not be able to do everyday tasks like driving or reading even with glasses.
Low vision affects millions of Americans — including many older adults. People with low vision aren’t blind, but because of their vision loss, they may not be able to do everyday tasks like driving or reading even with glasses.




 Don’t smoke. Smoking increases your risk for age-related macular degeneration, cataract, and other eye diseases and conditions that can damage the optic nerve.
Don’t smoke. Smoking increases your risk for age-related macular degeneration, cataract, and other eye diseases and conditions that can damage the optic nerve. Wear protective eyewear when outdoors. Protecting your eyes from the sun’s ultraviolet rays when you are outdoors is vital for your eye health. Wearing sunglasses that block 99 to 100 percent of both UV-A and UV-B radiation.
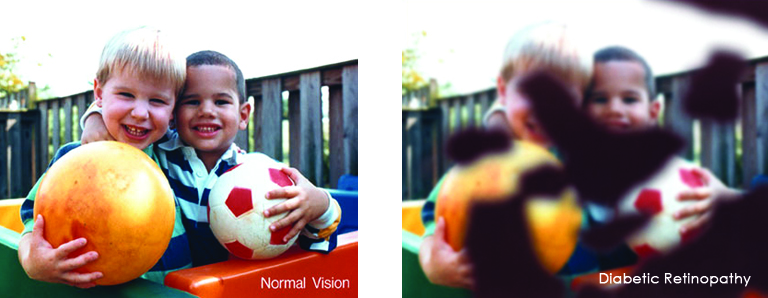
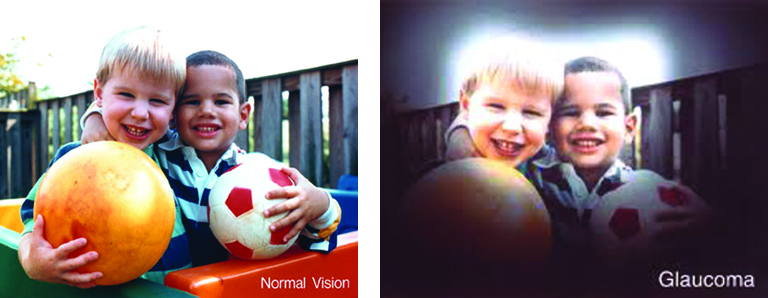
Wear protective eyewear when outdoors. Protecting your eyes from the sun’s ultraviolet rays when you are outdoors is vital for your eye health. Wearing sunglasses that block 99 to 100 percent of both UV-A and UV-B radiation. Know your family history. Talk to your family members about their eye health history. It’s important to know if anyone has been diagnosed with a disease or condition since many are hereditary, such as glaucoma, macular degeneration, and diabetes . This will help determine if you are at higher risk for developing an eye disease or condition.
Know your family history. Talk to your family members about their eye health history. It’s important to know if anyone has been diagnosed with a disease or condition since many are hereditary, such as glaucoma, macular degeneration, and diabetes . This will help determine if you are at higher risk for developing an eye disease or condition. Consider a multivitamin. Vitamins C, E and the mineral zinc have been shown to promote eye health. Vitamins with Lutein and Zeaxanthin have been known to help patients with moderate to severe age-related macular degeneration.
Consider a multivitamin. Vitamins C, E and the mineral zinc have been shown to promote eye health. Vitamins with Lutein and Zeaxanthin have been known to help patients with moderate to severe age-related macular degeneration. Give your eyes a rest. If you spend a lot of time at the computer or focusing at any one distance, you sometimes forget to blink, resulting in dryness and eye fatigue. Every 20 minutes, look away about 20 feet in front of you for 20 seconds. This can help reduce eyestrain. Consider using a lubricant eye drop during long periods of intense eye use and rest your eyes for 5 minutes.
Give your eyes a rest. If you spend a lot of time at the computer or focusing at any one distance, you sometimes forget to blink, resulting in dryness and eye fatigue. Every 20 minutes, look away about 20 feet in front of you for 20 seconds. This can help reduce eyestrain. Consider using a lubricant eye drop during long periods of intense eye use and rest your eyes for 5 minutes. Harsh weather conditions can reduce the natural moisture in your eyes and the irritation usually results in a burning or itching sensation that often leads to rubbing or scratching your eyes which can worsen the symptoms. Sometimes it feels like there is a foreign object in your eye and for some, dry eyes can even cause excessive tearing, as your eyes try to overcompensate for their lack of protective tears. Prolonged, untreated dry eyes can lead to blurred vision as well. Between the harsh winter winds outside and the dry heat radiating inside, our eyes are very quickly irritated and dried in the winter months. The result is itchy, dry eyes that may cause pain, blurred vision, a burning sensation, or even watery vision as our eyes try to compensate for the dryness.
Harsh weather conditions can reduce the natural moisture in your eyes and the irritation usually results in a burning or itching sensation that often leads to rubbing or scratching your eyes which can worsen the symptoms. Sometimes it feels like there is a foreign object in your eye and for some, dry eyes can even cause excessive tearing, as your eyes try to overcompensate for their lack of protective tears. Prolonged, untreated dry eyes can lead to blurred vision as well. Between the harsh winter winds outside and the dry heat radiating inside, our eyes are very quickly irritated and dried in the winter months. The result is itchy, dry eyes that may cause pain, blurred vision, a burning sensation, or even watery vision as our eyes try to compensate for the dryness.