 Recovering from eye surgery—whether it’s LASIK, cataract surgery, or retinal procedures—requires proper care to ensure the best results.Many patients underestimate how important post-operative care is; however, following the right steps can speed up healing and prevent complications.
Recovering from eye surgery—whether it’s LASIK, cataract surgery, or retinal procedures—requires proper care to ensure the best results.Many patients underestimate how important post-operative care is; however, following the right steps can speed up healing and prevent complications.
In this guide, we’ll cover the most important do’s and don’ts after eye surgery to help you protect your vision and recover safely. Additionally, these tips will support a smoother and more comfortable recovery process.”
Do’s After Eye Surgery
- Follow Post-Operative Instructions Carefully – Your ophthalmologist provides personalized instructions based on your procedure. These may include:
-
- Medication schedules
- Activity restrictions
- Eye protection guidelines
- Use Prescribed Eye Drops Consistently
Eye drops are essential for:
-
- Preventing infection
- Reducing inflammation
- Keeping the eyes moist
- Missing doses can delay healing and increase risks.
- Protect Your Eyes at All Times – After surgery, your eyes are more sensitive.
Protect them by:
-
- Wearing sunglasses outdoors
- Using protective shields while sleeping
- Avoiding dust and wind exposure
- Limit Screen Time – Digital screens can strain your eyes and slow recovery.
Try to:
-
- Take frequent breaks (20-20-20 rule)
- Reduce phone and computer usage
- Avoid prolonged reading
- Maintain Proper Eye Hygiene
-
- Wash hands before touching near your eyes
- Avoid contamination from towels or tissues
- Keep your surroundings clean
- Attend Follow-Up Appointments – Follow-up visits allow your doctor to monitor healing and catch complications early.
Don’ts After Eye Surgery
- Don’t Rub Your Eyes
Rubbing your eyes can:
-
- Damage healing tissues
- Disrupt surgical results
- Increase infection risk
- Avoid Water Exposure
Stay away from:
-
- Swimming pools
- Hot tubs
- Direct water spray in showers
- Water may contain bacteria that can cause infection.
- Don’t Wear Eye Makeup Immediately
To reduce risk, avoid makeup for at least 1–2 weeks to prevent irritation and contamination.
- Avoid Strenuous Activities—ask your doctor what is allowed
Heavy lifting and intense workouts can increase eye pressure and delay healing.
- Don’t Skip Medications
Even if you feel fine, stopping medication early can lead to complications.
- Don’t Drive Until Cleared
Blurred vision and light sensitivity are common after surgery. Only drive when your doctor approves.
How Long Does Eye Surgery Recovery Take?
Recovery time depends on the procedure:
-
- LASIK: 24–48 hours initial recovery
- Cataract surgery: A few days –2 weeks for functional vision
- Retinal surgery: Several weeks
Full healing may take longer depending on individual factors.
Signs of Complications After Eye Surgery
Contact your ophthalmologist immediately if you experience:
- Sudden vision loss
- Severe eye pain
- Increased redness
- Light flashes or floaters
- Eye discharge
Tips for Faster Recovery After Eye Surgery
- Stay hydrated
- Get enough sleep
- Avoid smoking and alcohol
Conclusion
Proper recovery after eye surgery is essential for achieving the best results. In fact, by following these do’s and don’ts, you can minimize risks, heal faster, and protect your vision long-term.
Always consult your surgeon if you’re unsure about any part of your recovery process.


 When we think about healthy eating, we usually picture stronger muscles, better digestion, or sharper memory. But your eyes? They’re often left out of the conversation — even though they depend on nutrients just as much as the rest of your body.
When we think about healthy eating, we usually picture stronger muscles, better digestion, or sharper memory. But your eyes? They’re often left out of the conversation — even though they depend on nutrients just as much as the rest of your body.


 Here are a few ways you can help protect your vision
Here are a few ways you can help protect your vision

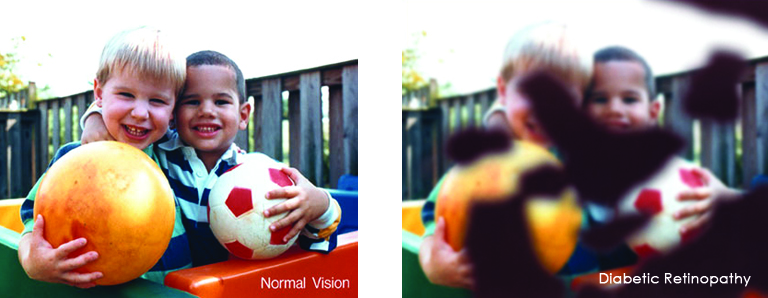
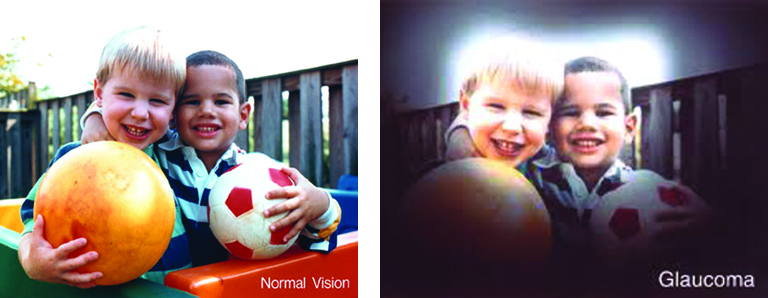
 Low vision affects millions of Americans — including many older adults. People with low vision aren’t blind, but because of their vision loss, they may not be able to do everyday tasks like driving or reading even with glasses.
Low vision affects millions of Americans — including many older adults. People with low vision aren’t blind, but because of their vision loss, they may not be able to do everyday tasks like driving or reading even with glasses.

 Understanding What 20/20 Vision Means
Understanding What 20/20 Vision Means