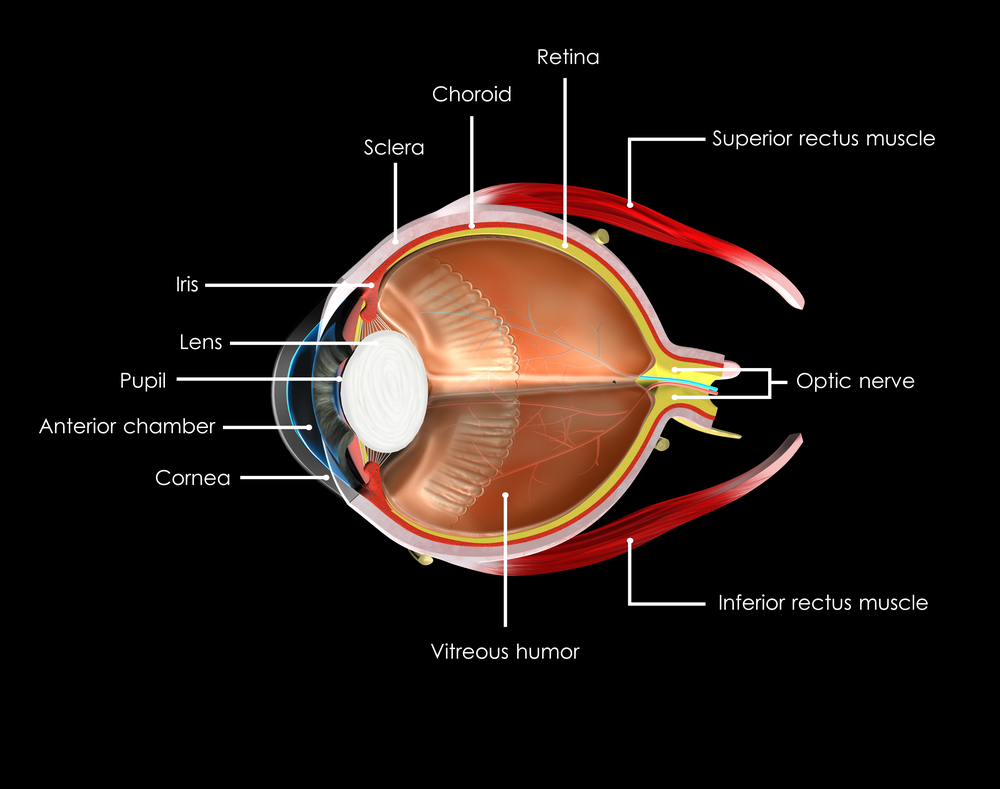
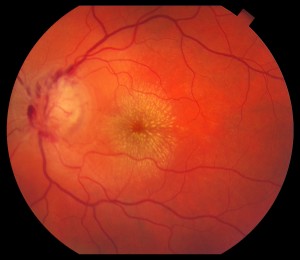
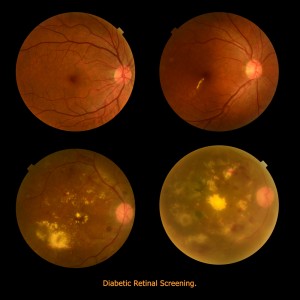
Ocular herpes is caused by the type 1 herpes simplex virus, and is a common, recurrent viral infection affecting the eyes. This type of herpes virus can cause inflammation and scarring of the cornea. Herpes of the eye can be transmitted through close contact with an infected person whose virus is active.
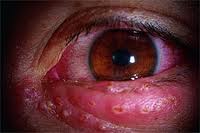
The National Eye Institute (NEI) says an estimated 400,000 Americans have experienced some form of ocular herpes, with close to 50,000 new and recurring cases occurring each year, ranging from a simple infection to a condition that can possibly cause blindness. There are several forms of eye herpes:
- Herpes keratitis is the most common form of eye herpes and is a viral corneal infection. Ocular herpes in this form generally affects only the top layer which is called the epithelium, of the cornea, and usually heals without scarring.
- Stromal keratitis occurs when the infection goes deeper into the layers of the cornea. This can lead to scarring, loss of vision and, occasionally, blindness. Although the condition is rare, the NEI reports that stromal keratitis is the leading cause of corneal scarring that subsequently causes blindness in the United States.
- Iridocyclitis is a serious form of eye herpes where the iris and surrounding tissues inside the eye become inflamed, causing severe sensitivity to light, blurred vision, pain and redness.
Treatment for eye herpes depends on where the infection is located in the eye – in the corneal epithelium, corneal stroma, or iris, etc.
Some ocular herpes treatments could aggravate the outbreak and therefore should be considered on a case-by-case basis.
If the corneal infection is only superficial, it can normally be alleviated by using antiviral eye drops or ointments, or oral antiviral pills over a two to three week period. In some patients, both drops/ointments and pills are used. Steroid drops can help decrease inflammation and prevent corneal scarring when the infection appears deeper in the corneal layers. Steroid drops are almost always used in conjunction with and simultaneously with antiviral drops. For those relatively few eyes where, despite the best of treatment, the virus has caused vision-impairing scars, corneal transplantation surgery is often a highly successful solution.
Although eye herpes has no cure, treatment can help control outbreaks. Studies are underway to determine better methods for managing the disease.
1/27/15
 Susan DeRemer
Susan DeRemer
Vice President of Development
Discovery Eye Foundation