12/18/14
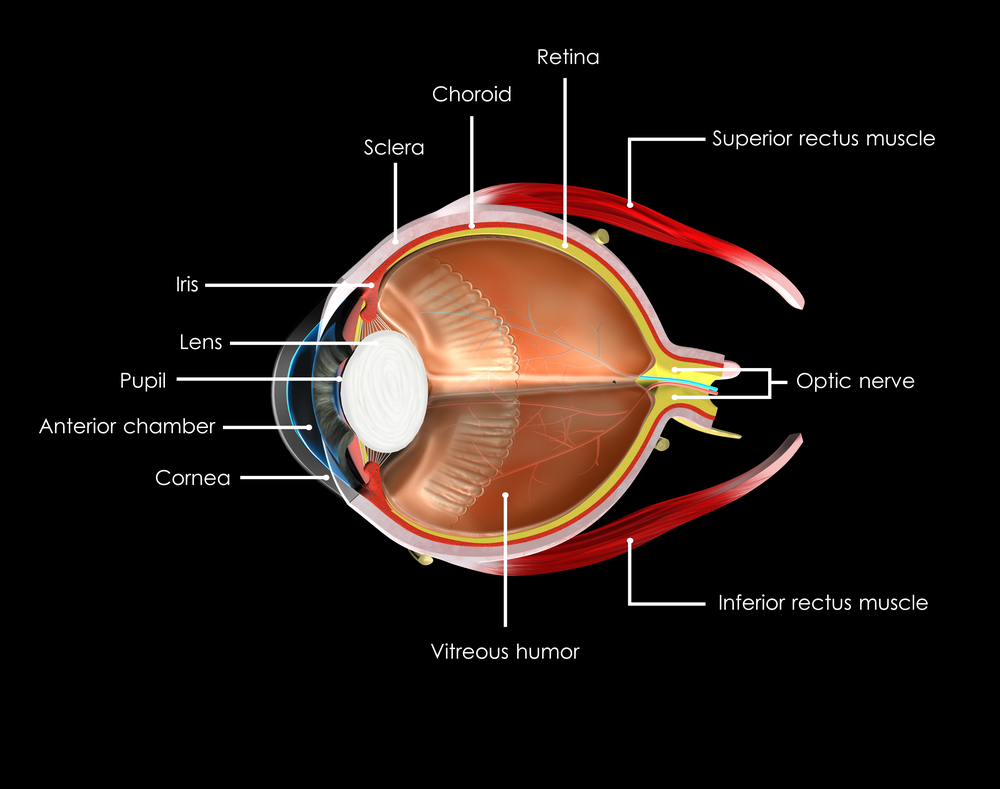
Uveitis is defined as inflammation of the uveal tissue. The uvea includes the iris, ciliary body, and the choroid of the eye. The iris is located in the anterior compartment of the eye and acts like the aperture of the camera, precisely filtering the amount of light entering the eye. The ciliary body, which is attached posteriorly to the iris, is involved in both the production of the aqueous fluid in the eye as well as the accommodation of the lens apparatus. The choroid is a dense layer of blood vessels that sits underneath the retina on the back wall of the eye, helping to nourish and remove metabolic waste products from the retina. Inflammation of any of these structures will consequently cause disruption of the visual pathway and over the long term can cause permanent visual loss. In fact, uveitis is the third most common cause of preventable blindness in the developed world.
Symptoms of uveitis include blurry vision, ocular pain, photophobia, redness, and floaters. These can be acute in nature, lasting a few days to weeks, and in some cases can be chronic, lasting weeks or months. Anyone with any of these symptoms should see their eye care provider as soon as possible, as faster treatment of uveitis has shown to result in better long term visual outcomes.
Uveitis can affect virtually any part of the eye, from front to back. Anterior uveitis or iridocyclitis is confined to the iris, ciliary body, anterior chamber, and cornea. Inflammation affecting the vitreous is termed intermediate uveitis, or pars planitis, and any inflammation affecting only the retina or choroid is termed posterior uveitis. The term panuveitis may be used when multiple layers of the eye are affected.
There are many possible causes of uveitis, including infection, inflammatory diseases, autoimmune diseases, and trauma. However, the majority of cases of uveitis, approximately half, are considered idiopathic, where no etiology is ever found. Trauma is the next most common cause of intraocular inflammation, accounting for approximately 20% of all cases. The remaining cases are secondary to a systemic disorder or localized ocular condition. Systemic etiologies can include inflammatory disorders such as sarcoidosis, infections such as tuberculosis and syphilis, as well as autoimmune diseases such as rheumatoid arthritis and lupus.
Treatment of uveitis is aimed at both blunting the intraocular inflammation as well as addressing any underlying systemic etiology. The most common treatment is the use of corticosteroids. These can be taken orally, or used topically as eye drops. In some cases, corticosteroids can be injected in or near the eye as well. If the uveitis is caused by an infection, such as tuberculosis or syphilis, the patient is also given antibiotics. Systemic corticosteroids can have major side effects when taken chronically, such as weight gain, hair loss, osteoporosis, hypertension, secondary diabetes, psychosis, and reduced growth in children. Because of these potential problems, the chronic use of systemic corticosteroids is not recommended. In cases of chronic uveitis that require long term treatment, immunosuppressive agents with less known side effects such as methotrexate, cyclosporine, and mycophenolate mofetil (Cellcept) are more commonly used. However, these biologic agents have their own set of potential side effects and therefore, it is recommended that a rheumatologist should also be involved in the care of the patient when using these agents. Topical and intraocular steroids localized to the eye can cause elevated intraocular pressure as well as cataracts. In most cases, elevated intraocular pressure can be controlled with topical glaucoma drops, but in some cases surgical intervention is required to prevent severe glaucomatous damage.
The most common type of uveitis is acute anterior uveitis or iridocyclitis. Many cases of anterior uveitis are idiopathic though almost half of all cases are associated with the HLA- B27 haplotype. Systemic diseases associated with HLA-B27 include psoriatic arthritis, ankylosing spondylitis, reactive arthritis, and inflammatory bowel syndrome. Signs of anterior uveitis include redness of the eye, sometimes termed ciliary flush. The conjunctiva can become extremely red, and when associated with ocular pain and photophobia, is a strong indicator of anterior uveitis. Inflammatory cells found in the anterior chamber are the hallmark of anterior uveitis, sometimes deposited on the corneal endothelium (keratic precipitates) or iris (Bussaca nodules). Patients with anterior uveitis are typically treated with topical corticosteroid and cycloplegic eye drops. A laboratory workup for systemic etiologies is usually not necessary unless the patient experiences a recurrent episode.
Inflammation affecting primarily the vitreous cavity is known as intermediate uveitis or pars planitis. Inflammatory cells in the vitreous, known as vitritis, are typically bilateral, and when severe, can be found clumped in the vitreous cavity (snowballs) or deposited on the inferior pars plana (snowbanking). Intermediate uveitis is typically idiopathic though sarcoidosis, multiple sclerosis, and Lyme disease are also possible causes. Certain malignancies such as lymphoma can also ‘masquerade’ as intermediate uveitis, and when seen in older patients, should be suspected and ruled out.
Posterior uveitis involves the retina, choroid, and/or the retinal vasculature, and usually is more difficult to treat than anterior uveitis.
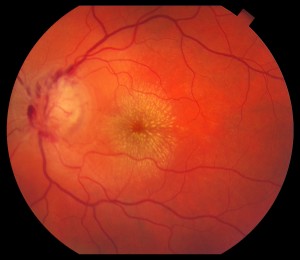
In many cases, patients with posterior uveitis will exhibit characteristic exam findings that help narrow the differential diagnosis. For instance, an area of active retinitis next to an old pigmented chorioretinal scar is highly suggestive of toxoplasmosis. The most common symptom in patients with posterior uveitis is blurred vision. One of the more typical findings in posterior uveitis is macular edema, which is usually treated with periocular or intraocular corticosteroids.
In summary, uveitis is a visually threatening inflammatory condition that should be diagnosed and treated immediately. It is important to determine as best as possible the etiology of the uveitis and treat appropriately. In general, most patients with uveitis have good visual recovery with the proper management. However, in some cases, severe damage can occur, either due to the inflammation itself (usually chronic) or as a side effect of therapy (corticosteroids).
 Richard H. Roe, MD, MHS
Richard H. Roe, MD, MHS
Retina-Vitreous Associates Medical Group

