This article is reprinted with the permission of Dr. Kenneth W. Wright, Medical Director of the Wright Foundation for Pediatric Ophthalmology & Strabismus. Check out his website for information on over 20 pediatric eye disease and conditions.

Normal Binocular Vision
Normally, both eyes are aligned on the same visual target and the images from each eye are merged in the brain to form a single three-dimensional image, or binocular vision. The brain’s process of merging or “fusing” images from each eye into one image is called binocular fusion. The perception of three-dimensional depth is called stereoscopic vision. Stereoscopic vision is the highest level of binocular vision and requires intricate processing of information from both eyes. Binocular vision develops during early infancy, and proper alignment during this time is necessary for normal binocular development to occur.
Accommodative Esotropia
Esotropia means one eye is turned in towards the nose, or crossed eyes. Patients with esotropia have one eye aligned on the visual target, but the other eye is turned in towards the nose. When the eyes are crossed only one eye is aligned with the target and the child is forced to use only one eye for vision. Accommodative esotropia is a type of esotropia caused by significant farsightedness (hypermetropia). Most think that farsighted people can see well only in the distance. In children, this is not true. Children have the ability to focus great amounts, so most children can see well for distance and near even without glasses. Focusing (medically termed accommodation) is the process of increasing the lens power of the eye to see clearly. Linked to focusing is the natural reflex of convergence (eyes move in). As one focuses on an approaching near object, the eyes move in to stay on target. This process of focusing and convergence used for near vision is termed the near reflex. Accommodative esotropia occurs because the farsighted child has to over focus to see clearly. When eyes over focus, the natural reflex is for the eyes to cross. You can experience this by trying to see the tip of your nose. When you look at the tip of your nose you have to over focus and consequently your eyes cross. Since more focusing is needed to see near objects, the crossing tends to be greater when looking at close objects.
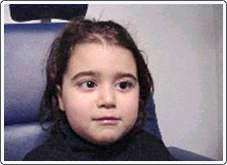
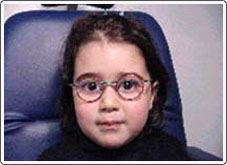
The onset of accommodative esotropia is most commonly seen between the ages of 2 and 4; however, even infants can have crossed eyes. This situation is usually first noticed when the child is tired, sick, or looking at an object very near to their face. Some children cross when they are tired and this is because they cannot sustain the effort to keep the eyes straight. The crossing is usually intermittent at first, but can quickly become constant. There may be a parent or a close relative with the same problem; however, in many cases there is no family history of crossed eyes.
During the examination, three important determinations are necessary. The first determination is to make sure the vision is normal in each eye. This is done by assessing the visual behavior of the preverbal child, or simply having the verbal child read the eye chart. Secondly, the amount of crossing is evaluated. This is measured using prisms while the child is viewing an object. Thirdly, the need for glasses is measured, and this requires drops to dilate the pupil and relax the child’s focusing. These drops take approximately 20 to 30 minutes to work and will blur vision for 1 to 3 hours, but the pupil may stay large for much longer. After the eyes have been dilated, the eyeglass prescription is calculated using a special light (retinoscope) along with lenses. Determining the proper lens power in young children is difficult and may require repeat exams and changes in the eyeglass lenses.
Effects of Esotropia on Visual Development
Esotropia occurring in young children and infants results in the immature brain turning off the information from the deviated eye. This mechanism of turning off visual areas of the brain connected to the deviated eye is called “suppression.” Thus, patients with esotropia use one eye at a time (monocular vision) and do not have binocular fusion or stereoscopic vision. Suppression disrupts normal binocular visual development and if not treated early, causes permanent loss of binocular vision and stereoscopic vision. Early treatment of esotropia is critical to stimulate binocular development.
How Do Patients with Esotropia See?
If the esotropia is acquired in late childhood (after 7 to 9 years of age) or in adulthood, it will cause double vision. Esotropia occurring in infants and young children, however, does not cause double vision, as the young, immature brain has the ability to suppress the information from the deviated eye. The child uses one eye at a time to see and avoids double vision. The fact that the eyes are crossed disrupts normal binocular visual development and often causes permanent loss of binocular vision and stereoscopic vision. Early treatment of esotropia is critical in order to stimulate binocular development.
Treatment of Accommodative Esotropia
Glasses
The goal of treatment is to align the eyes, stimulating them to work together to establish binocular vision and stereoscopic vision. Children and infants who are significantly farsighted are best treated with glasses. If the glasses align the eyes, then surgery is not necessary, and the treatment is to continue with the glasses. The full, hypermetropic (farsighted) prescription is usually given via eyeglasses, and most parents are surprised at how well these children adjust to the glasses. When properly worn, most children adapt to the glasses like “fish to water.” The glasses not only straighten the eyes, but also relax the child’s vision, as they no longer have to over focus. In patients with accommodative esotropia, glasses must be worn full-time. Older children over 4 to 5 years may have blurred distance vision when they first put on their glasses. This is because they had a strong habit of over-focusing and continue to do so even when wearing the glasses. Over several days, most children will relax their over-focusing and enjoy the comfort the glasses afford. In those children who do not adapt to the glasses, drops can be used to relax focusing, or a reduced prescription power can be given. In most cases, however, the best treatment is to give the full power. The eyes usually straighten within a few days to a few weeks after wearing the glasses. If the eyes are still crossing with the glasses and the child is not using the eyes together after several weeks, then eye muscle surgery is usually required. Occasionally, an initial response to glasses is that the eyes “break down” and cross for distance and near. In this situation, surgery in addition to the glasses may be required.
Bifocal Glasses
In certain children, glasses will align the eyes for distance viewing, but the eyes will still cross for near work. These patients can be helped with bifocal glasses. A bifocal is a small powerful lens placed in the lower part of the eyeglass lens. This more powerful lens will further relax near focusing to straighten the eyes for near work. Chin-up posturing for near work indicates that the child is using the bifocals correctly and is viewing through the bifocal lens for near work.
Amblyopia
Some children with crossed eyes have a strong fixation preference for one eye (dominant eye) and constantly have one eye turned in. Constant use of only one eye can lead to vision loss of the deviated, or non-dominant, eye. Poor vision occurs as visual areas in the brain connect with the dominant eye and are then subsequently suppressed. If left untreated, the deviated eye will progressively lose vision over time. This poor vision caused by brain suppression is called amblyopia. Amblyopia occurs only in young children when the visual areas are immature and still developing. Children who have a difference in the strength of the glasses in one eye as compared to the other have an increased risk of developing amblyopia in the more farsighted eye. Approximately 20 to 40% of patients with esotropia will also have amblyopia of the non-preferred eye.
Patching
If amblyopia is present, patching of the good eye is indicated to promote visual stimulation of the amblyopic eye and improve vision. Patching does not straighten the eyes and is not indicated if vision is equal. Another way to promote stimulation of the amblyopic eye is to blur the vision of the “good eye.” This can be done by placing a blurring lens over the good eye, or by administering drops to blur the good eye. In most cases, patching the good eye with an adhesive patch is the most practical treatment. Patching is continued until vision improves in the weaker eye, usually taking a few weeks to several months. In the vast majority of patients, vision can be improved if the parents and child are compliant with the treatment.
10/8/15
 Kenneth W. Wright, MD
Kenneth W. Wright, MD
Medical Director, Wright Foundation for Pediatric Ophthalmology & Strabismus
Clinical Professor of Ophthalmology, USC Keck School of Medicine

